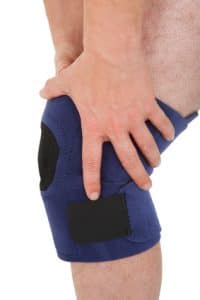
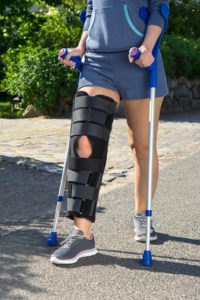
After a serious injury, your doctor often will recommend that you have surgery to have the best recovery. Unfortunately, getting that surgery done is not always easy in a workers compensation case.
Many people get frustrated because they run into the problem when the workers compensation insurance company will not approve the surgery. If you find yourself in this or a similar situation, you probably have some questions:
- Does workers compensation require the insurance company to pay for surgery?
- What can you do if the insurance company does not meet its obligation of paying for surgery?
I talk to many people who find themselves in this situation. This article will provide helpful information about getting the insurance company to authorize workers compensation surgery and some of the pitfalls you should watch out for.
 What types of surgery does Georgia workers compensation cover?
What types of surgery does Georgia workers compensation cover?
The first question many people have is whether Georgia’s workers compensation laws require the insurance company to pay for surgery. To answer that question, we need discuss what workers compensation covers regarding medical treatment.
Generally, the law in Georgia requires the workers compensation insurance company to pays for the medical treatment and testing that you need as a result of your injury at work.
Surgery is often a type of medical treatment that you need because of your injury at work. Many injured workers need surgery to repair herniated disc, torn ligaments, or broken bones.
There are some special rules about workers compensation medical treatment. One special rule is that you cannot just have surgery with any doctor you want. The doctor performing treatment has to be an authorized physician. So, the doctor must either be your authorized treating physician or a doctor to whom your authorized treating physician referred you.
Another special rule is that the treatment must be reasonable and necessary and related to your workers compensation injury. If the surgery does not meet these requirements, then the insurance company will not have to pay for it.
If I am seeing a workers compensation doctor, why does the insurance company not just approve my surgery?
If you have had an injury at work, there is a good chance the workers compensation insurance company has caused you some frustration. If you are at the point where your doctor is recommending surgery, then you probably have waited several months going through nonsurgical treatment and testing.
Now, your doctor is saying you need surgery in order to have a full recovery from your injury. So, you may be a little bit frustrated but also a little bit hopeful that you are going to get that surgery done, recover from it, and then be able to move on with your life.
Unfortunately, just because your doctor recommends surgery does not mean that that surgery is going to be approved by the insurance company. Insurance companies often delay or deny approval of workers’ compensation surgery. They do this in a few different ways:
One is just by not answering the doctor’s office when they ask for approval. So they do not provide an answer one way or another. This often leaves the doctor’s office very frustrated.
Your doctor wants to know that they are going to get paid for the surgery after they perform it. Because of this, doctors almost never perform workers compensation surgery unless they have approval from the insurance company. So, when the insurance company does not answer and give approval, your surgery gets delayed.
A second way the insurance company delays treatment is by saying that you need a second opinion or that they need more information before they can approve the surgery.
A third way the insurance company delays treatment is just by denying the surgery completely. They tell the doctor they are not going to approve it or they may file a form called a WC-3 controvert denying the surgery.
So what can you do if your surgery is being delayed or denied?
Delay is almost never good for you when you are injured. So, you probably want to get your surgery approved as quickly as possible.
The first thing you can do is reach out to the insurance company. You could speak with the adjuster or case manager and ask that they approve the surgery.
If this works, great. You can move forward and have the surgery. Unfortunately, this does not often work.
A second option that’s available if this does not work is to use one of the forms that is published by the Georgia State Board of Workers’ Compensation to try to make medical treatment get approved faster.
One of these forms is called a WC-205. That is a form that your doctor’s office can use to request approval for the surgery.
Your doctor’s office can complete and submit the Form WC-205 to the adjuster. The adjuster has a certain amount of time to respond either approving the surgery or denying the surgery. If the adjuster does not give any answer at all within the time allowed, then the surgery should be deemed approved.
A second form that can be used by you or your attorney is called a Form WC-PMT. The intent of this form is to allow you to set up a conference call with a workers compensation Administrative Law Judge.
 In this conference call, the judge will discuss whether the requested medical treatment should be approved. When you file a WC-PMT about surgery, the WC-PMT call can result in an order from the judge approving the surgery.
In this conference call, the judge will discuss whether the requested medical treatment should be approved. When you file a WC-PMT about surgery, the WC-PMT call can result in an order from the judge approving the surgery.
When the Form WC-PMT is completed and submitted to the insurance company, the insurance company should either file a response approving the requested medical treatment or denying the requested medical treatment. If they do not do anything, then the conference call with the judge will take place.
What can you do if these tactics to get your surgery approved do not work?
If you cannot get your surgery approved, you could also try other ways of getting your case in front of a judge. You could file a Form WC-14 to request a hearing in front of a workers compensation judge. You could also file a motion to try to get treatment approved.
The best approach to getting your surgery approved depends on the specific facts of your case. Sometimes, a motion is the best approach. In other situations, a hearing request is the best choice.
At a hearing, you or your attorney can try to prove that you should have the surgery that has been recommended as a result of your injury at work. I would certainly recommend that if you were going to go to court about your case that you talk to an attorney and hopefully hire an attorney to represent you.
Workers compensation court has very specialized rules. If you do not understand these rules, there is a good chance that you will lose your case because the judge will not consider all the evidence needed to prove your case.